May 1, 2015
What’s Good for Moms is Good for Their Babies:
Addressing Postpartum Depression in the Pediatrician's Office
Maternal mental health plays a critical role in children’s healthy development. Infants need to be nurtured from the start of life in order to thrive. Unfortunately, many new mothers struggle with postpartum depression or other serious mental health challenges but very few get the support and treatment they need. Up to 22 percent of the four million women who give birth each year in the United States experience postpartum depression that can interfere with early parenting. Of Connecticut’s approximate 37,000 births in 2014, this translates to as many as 8,000 mothers per year. Yet research shows that fewer than half of all affected mothers receive a mental health diagnosis and only 15% of those who do receive a diagnosis seek mental health services.
Helping Babies Thrive
Child health providers who have frequent contact with mothers of infants, often do not recognize that women are suffering. Failure to identify mothers with mental health disorders and connect them to helpful interventions is an enormous missed opportunity to ensure the healthy development of children.
Pediatricians are well positioned to help. Newborns and their mothers visit pediatric providers routinely in the baby’s first year of life (typically six times in the first six months). The American Academy of Pediatrics encourages universal surveillance and screening for postpartum depression. By using standardized brief screening tools – often two questions - during an infant’s well-child visit, child health providers can identify mothers who need help and connect them to mental health services. The two-question screen asks about diminished mood and pleasure.
Advancements in neuroscience underscore the importance of healthy caregiver-infant interactions. Infant brain development relies on a concept called “serve and return.” The baby “serves” a sound, look or movement and relies on the caregiver to “return” with an appropriate response such as eye contact, words or a hug. Mothers who are depressed may have difficultly in being present in this way for their infants, which can disrupt their baby’s development. Identifying symptoms of depression in new mothers and connecting them to effective treatment can result in improved outcomes for the mother and her baby.
CHDI’s 2014 IMPACT Addressing Maternal Mental Health in the Pediatric Medical Home  reviews the most common types of maternal mental health disorders, how they affect child health and development, available treatments and the role of child health providers in early detection and linkage to services. This report provides an update to a 2008 IMPACT, which helped spark statewide improvement in early detection and treatment for mothers, as well as expansion of interventions for children.
reviews the most common types of maternal mental health disorders, how they affect child health and development, available treatments and the role of child health providers in early detection and linkage to services. This report provides an update to a 2008 IMPACT, which helped spark statewide improvement in early detection and treatment for mothers, as well as expansion of interventions for children.
Statewide Solutions
Connecticut has resources and policies in place to support screening in pediatric primary care and help providers connect mothers in need to services and effective treatment. In 2013, Medicaid approved reimbursement for pediatric providers to screen mothers as part of well-child visits and commercial insurers followed their lead. At the same time, CHDI began offering free training for pediatric health providers through our Educating Practices In the Community (EPIC) program. Training helps providers address postpartum depression by providing screening tools, billing codes and local treatment referral sources. Since 2013, CHDI has trained 136 pediatric health providers in Connecticut to address postpartum depression. The training offers pediatricians Continuing Medical Education credits and the opportunity to earn Maintenance of Certification credits.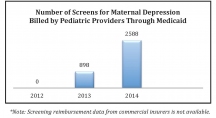
As a result of these financial and training supports, screening rates for postpartum depression are now on the rise across Connecticut, having nearly tripled in the past year.
Despite this progress, neither early detection nor treatment happens routinely. To efficiently and effectively reach the estimated 8,000 mothers experiencing maternal mental health disorders in Connecticut, child health sites need continued support. A full list of recommendations to improve perinatal mental health policy, practice and service delivery in Connecticut can be found in CHDI’s recent IMPACT.
For more information, contact Lisa Honigfeld at honigfeld@uchc.edu, 860-679-1523, visit www.chdi.org, or download CHDI’s IMPACT. Pediatric health providers can sign up for free training on postpartum depression at www.chdi.org/epic.